One Platform That Meets Your Practice Where You Are
Every practice runs PA differently. Maybe you have a dedicated coordinator, maybe your office manager handles it, maybe the clinician is doing it all. VerityAuth adapts to how your team actually works.
The PA Coordinator
Day-to-day PA workflow
The Practice Leader
Operations & revenue oversight
The Clinician
Clinical decisions & patient care
Handle Twice the Volume. Lose Zero PAs.
Whether it’s a dedicated coordinator or the office manager wearing another hat, whoever handles your day-to-day PAs is juggling 30+ active cases across multiple payers. Their day is phone calls, fax follow-ups, and status tracking — the same work that makes it impossible to appeal denials. VerityAuth gives them a command center that replaces the spreadsheet, the sticky notes, and the mental juggling — so when a denial comes in, they have the time and the tools to fight it.
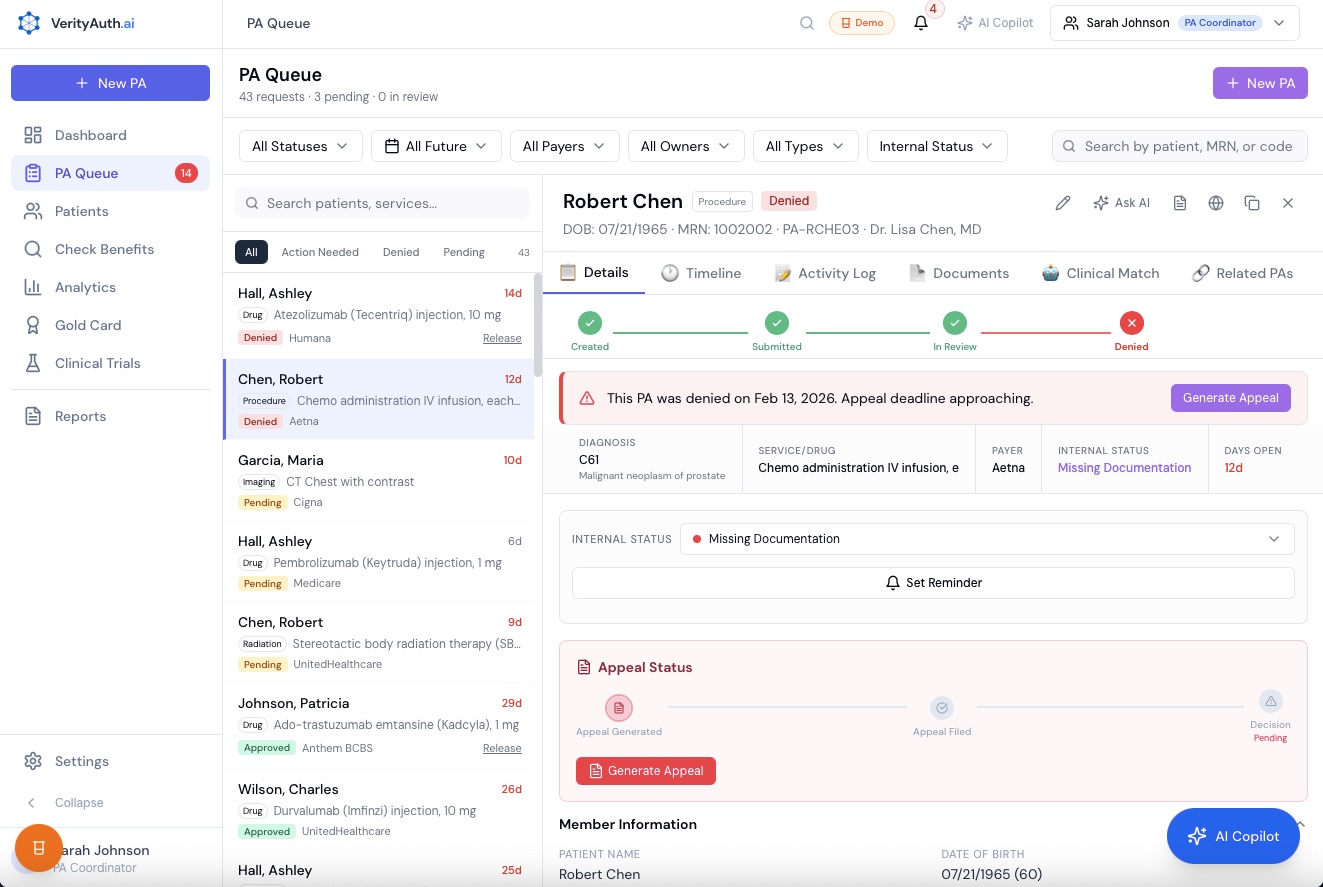
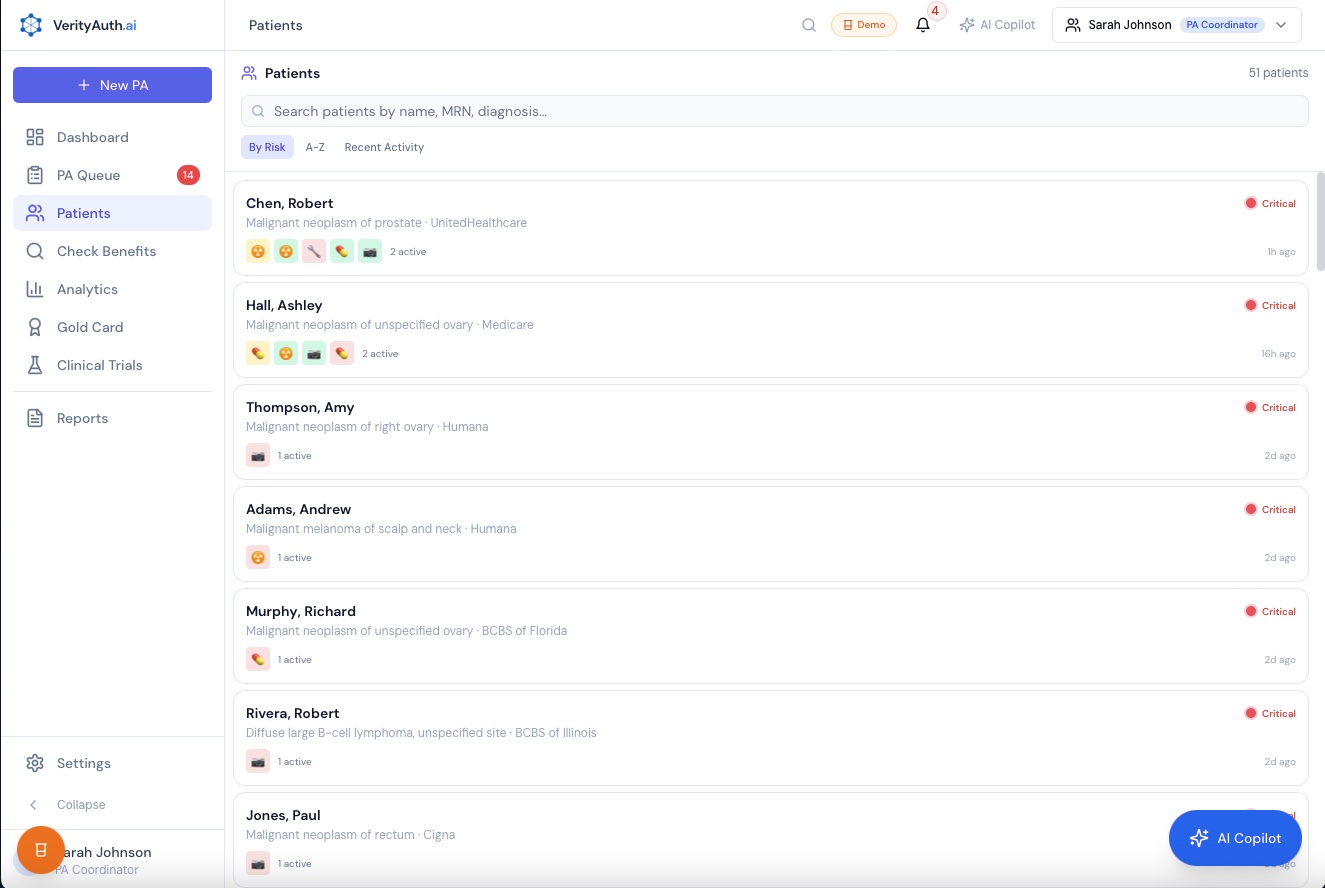
Patient View
All PAs for one patient grouped together. Risk indicators, active cases, and diagnosis at a glance.
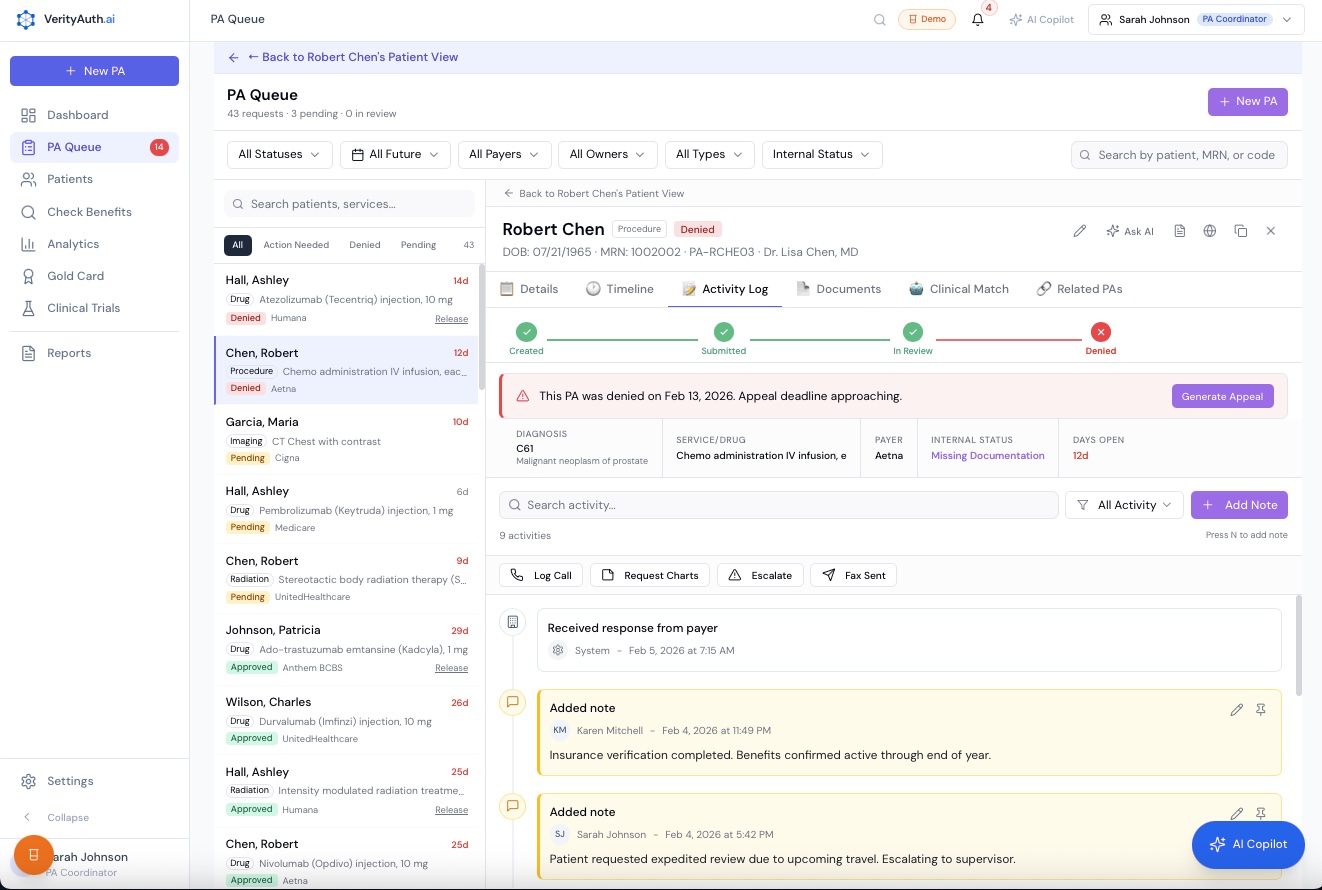
Activity Log
Full timeline for every PA. Who called, when, what happened. No more “did we hear back?”
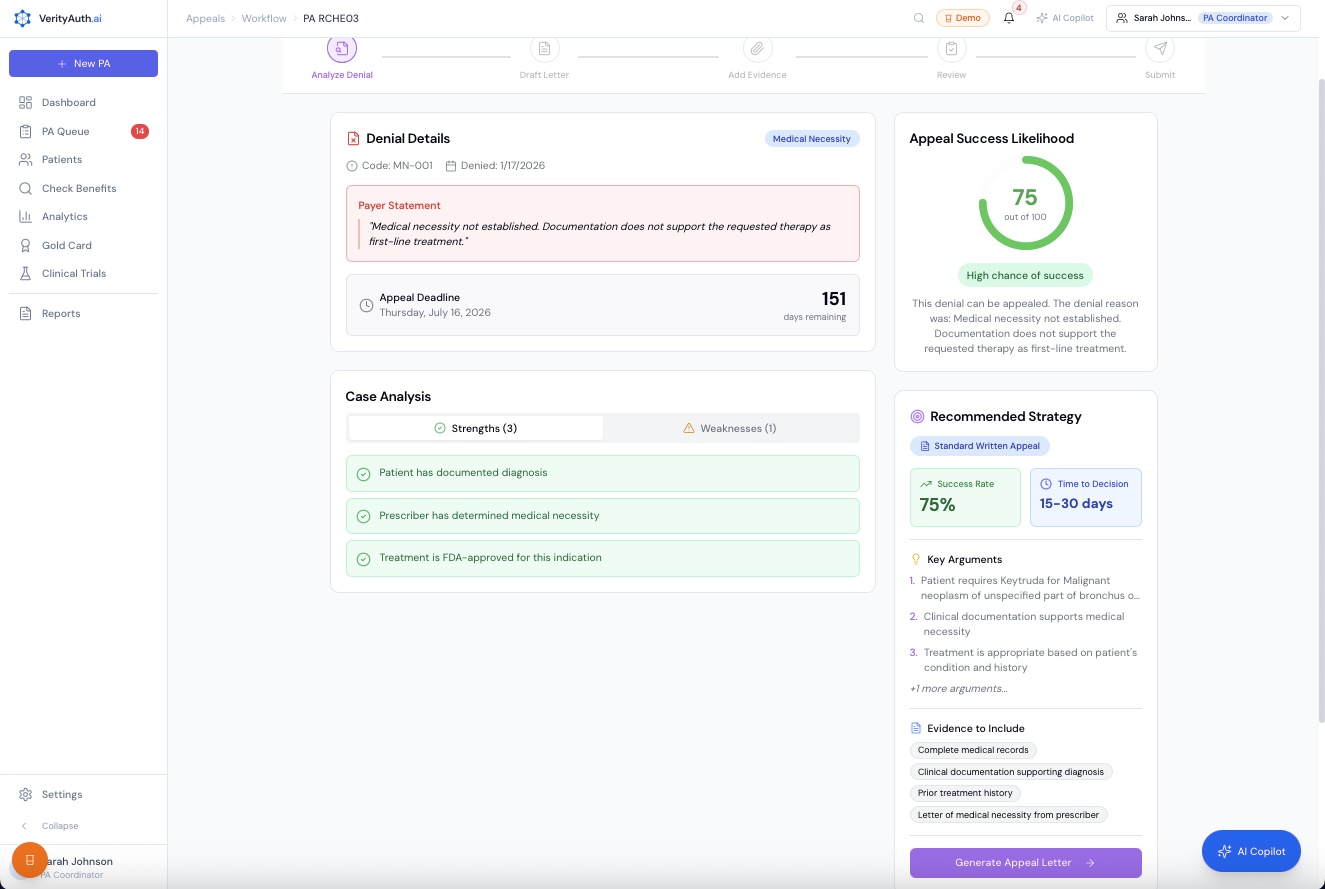
Appeal Generator
AI analyzes the denial, scores success likelihood, builds the case, and writes the letter. You click send.
See Where You’re Losing Revenue. Recover It.
Someone in your practice needs the big picture: are we keeping up? Who’s overloaded? Which payers are slow? Whether that’s an office manager, a practice administrator, or the lead physician — they need to answer one question above all: how much revenue are we losing to unappealed denials? VerityAuth answers it in real time and gives them the tools to turn lost revenue into recovered revenue.
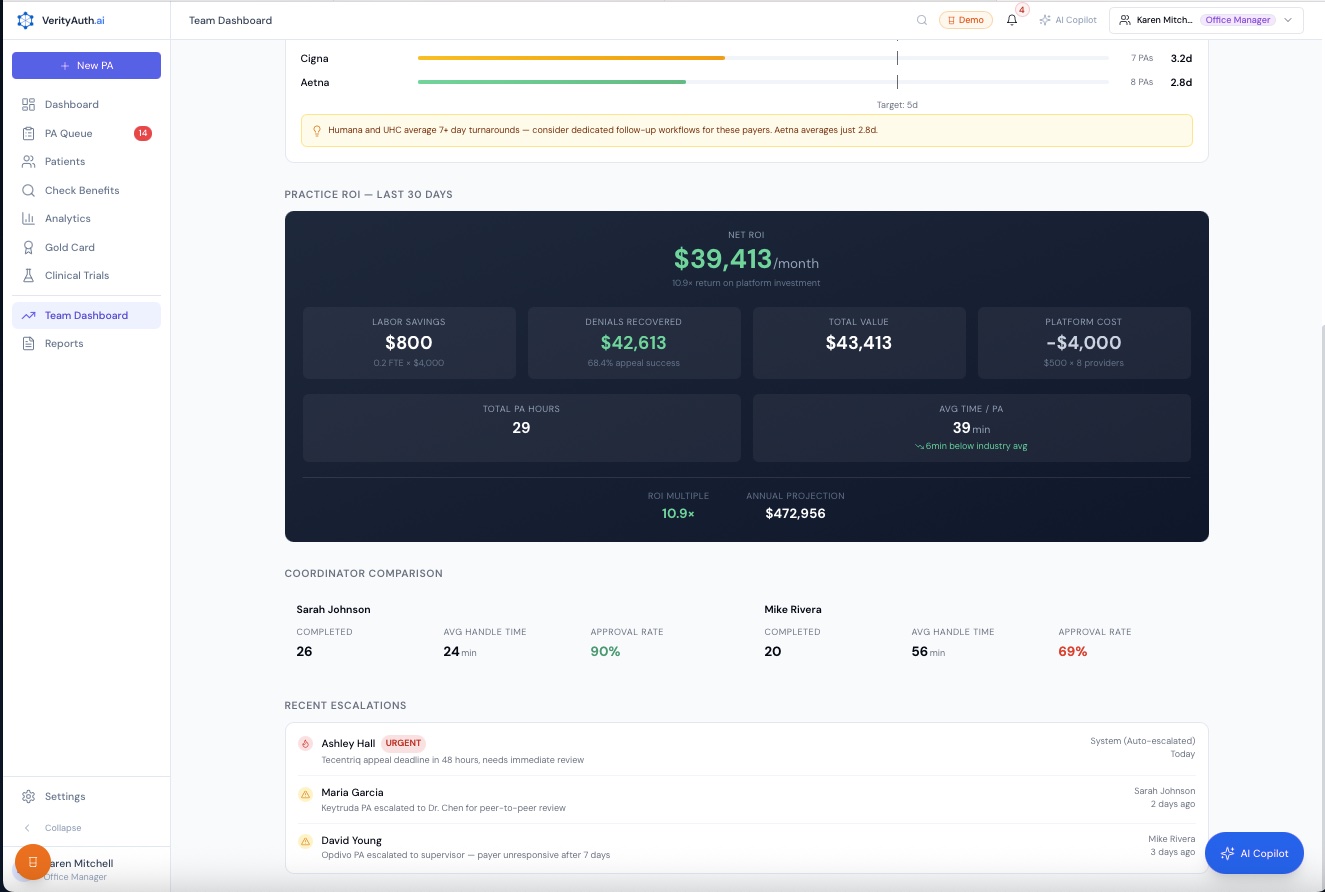
Revenue Recovery
Denials recovered, labor savings, ROI multiple, annual projections. The math that justifies the investment.

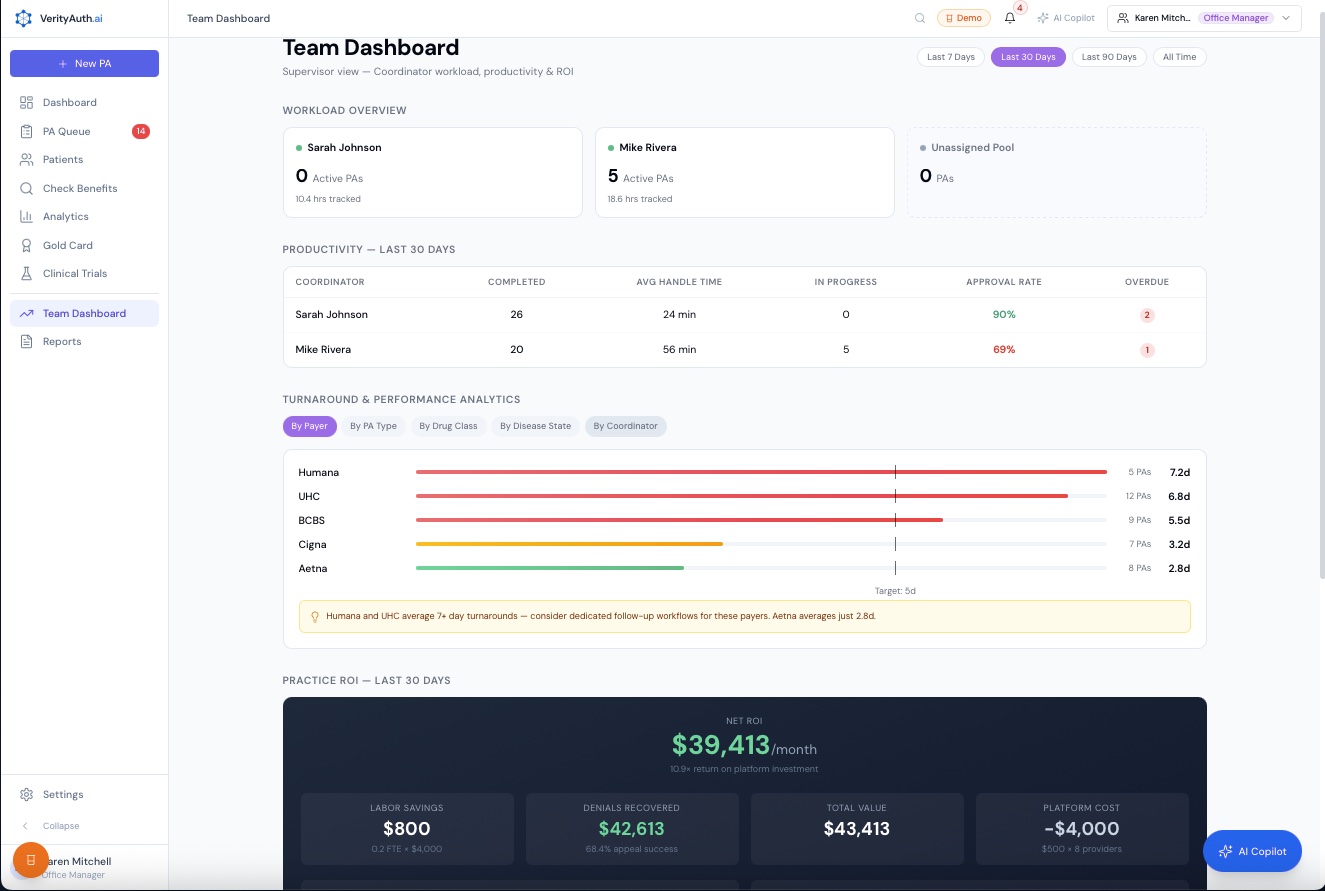
Team Performance
PA volume by coordinator, average turnaround, workload distribution. Staff where the volume is.
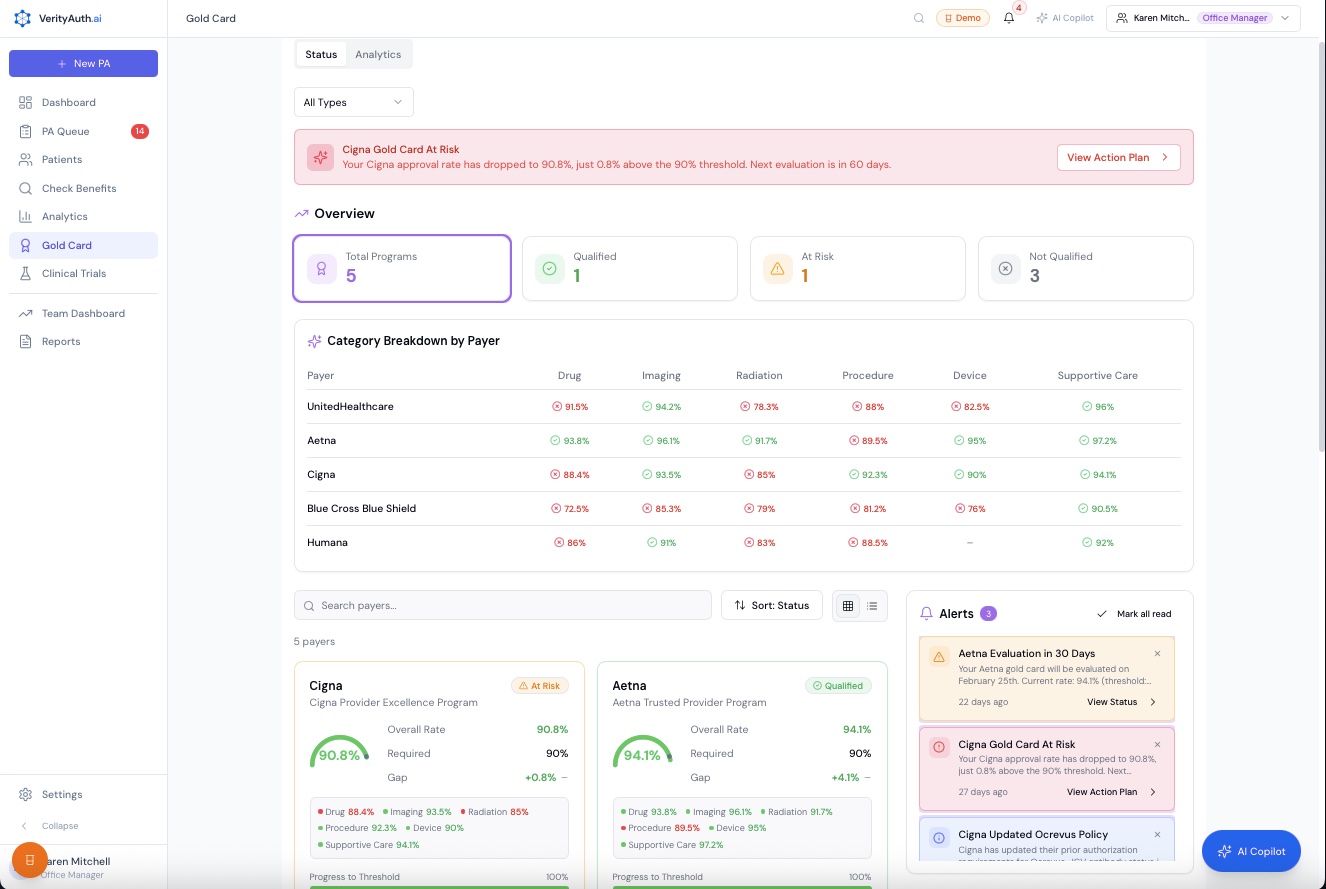
Payer Intelligence
Gold card tracking, approval rates by payer and category, and alerts when thresholds are at risk.
Your Patients Get the Treatment You Prescribed
Dr. Chen prescribes Keytruda because it’s the right drug for her patient. She shouldn’t have to wonder whether a payer will override her clinical judgment — and she definitely shouldn’t have to accept it when they do.
93% of oncologists report patients being forced onto second-choice therapy because of PA. Cancer Therapy Advisor Research shows that even 1–3 week delays in starting guideline-based treatment correlate with worse disease control and lower survival. Johns Hopkins Medicine
The system is overriding your clinical judgment, and your staff doesn’t have the time to fight back. VerityAuth fights back for you. Every denial appealed with NCCN-cited evidence. P2P talking points ready when the medical director calls. Your patients get what you prescribed — not what the payer’s algorithm substituted.
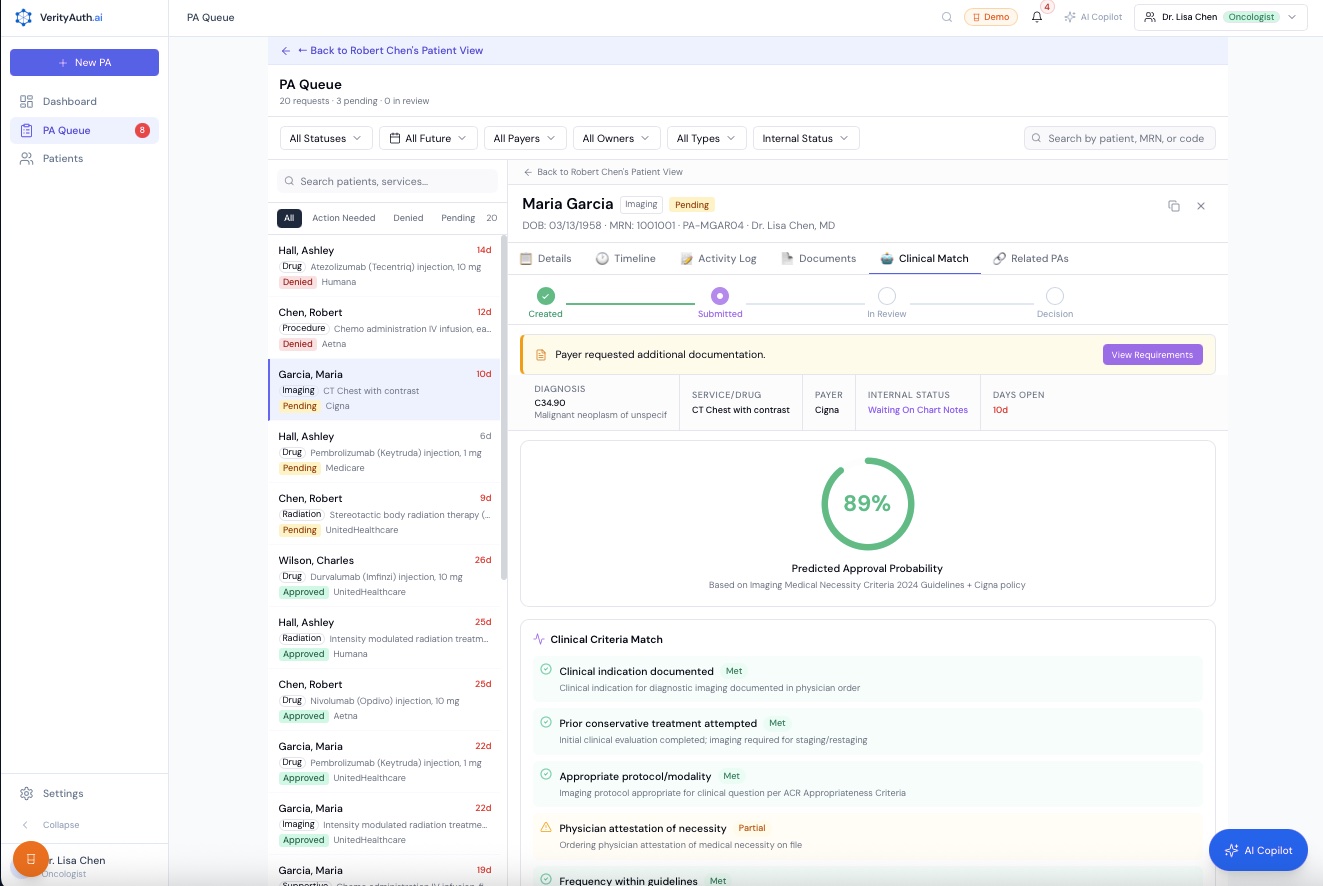

P2P Preparation
Clinical criteria matching with evidence citations specific to the patient’s regimen, stage, and biomarkers.
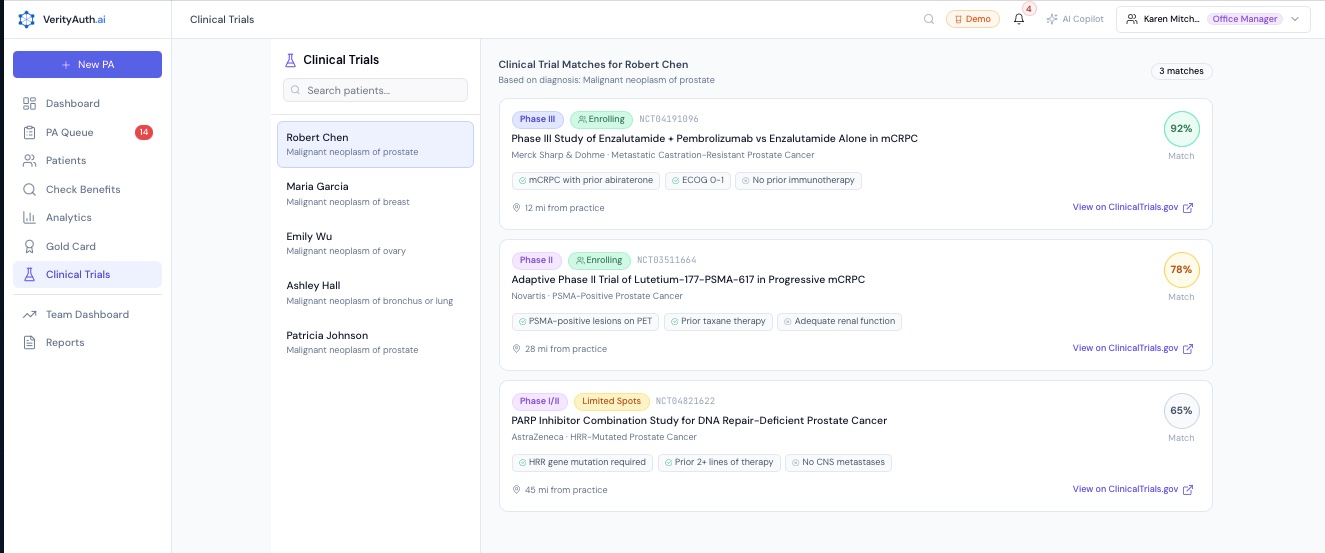
Clinical Trial Matches
Eligibility scoring, distance filtering, and one-click sharing when the appeal path closes.

Appeal Intelligence
Case strength analysis, key arguments, and evidence recommendations — so your P2P call is airtight.